In the U.S. healthcare sector, sensitive medical records are often subjected to cyberattacks like data breaches and ransomware. For example, recently a misconfigured MongoDB database has led to the exposure of 2.7 million patient profiles. This incident is due to a lack of security controls like strong passwords and authentication measures. Moreover, the reports from the Department of Health and Human Services say that the number of data breaches affecting 500 or more people is increasing every month. Such incidents could be avoided if business entities strictly implemented the HIPAA omnibus rule of 2013. But what is the HIPAA omnibus rule all about?
The Health Insurance Portability and Accountability Act (HIPAA) was enacted in 1996 to safeguard the sensitive patient records called protected health information (PHI). But, as discussed earlier, the security incidents in the healthcare sector have spiked in the last decade. Just one wrong click or a misconfiguration in cloud setup is enough to lose medical records online. Not to forget, attacks nowadays target all healthcare firms irrespective of their size. This is when the regulators understood that HIPAA needed a major upgrade. Hence, the HIPAA omnibus rule came in with major changes in regulations. These changes inform how healthcare entities should manage their data security and privacy. Compliance with the omnibus rules HIPAA is no longer optional for business associates handling electronic protected health information (ePHI)
This rule is more important now than ever. It has widened the scope of HIPAA rules by including business associates alongside healthcare providers under compliance regulations. Additionally, it gave the patient more power and rights regarding their ePHI. Therefore, this blog helps businesses to gain a complete understanding of the HIPAA omnibus rule and what the steps and practices are to implement them.
Tl; DR:
Concern: Cyberattacks on healthcare systems are rising, exposing sensitive patient data. A lack of strong security controls and outdated HIPAA enforcement has left many organizations—especially third-party service providers—vulnerable and non-compliant.
Overview: The HIPAA Omnibus Rule, introduced in 2013, updated the original HIPAA law. It closed major gaps by extending compliance obligations to business associates and subcontractors. It also gave patients more rights, introduced stricter breach reporting rules, and raised the penalties for violations.
Solution: To comply, healthcare organizations and their partners must update their Business Associate Agreements (BAAs), tighten data security policies, and implement best practices like regular HIPAA risk assessments, audit trails, and access controls. CertPro helps organizations navigate these changes by providing expert compliance guidance tailored to their size, risk, and budget.
UNDERSTANDING THE HIPAA OMNIBUS RULE
The HIPAA omnibus rule emerged as an update to the HIPAA regulations in 2013. It was introduced to improve the efficiency of data security and privacy in the U.S. healthcare system. To put it simply, the HIPAA omnibus rule gave more protection to the patients and added additional responsibilities to the healthcare providers and business associates.
Meanwhile, something unexpected was happening in the healthcare industry. The explosion of data breaches and changes in their business operations made older privacy laws less effective. To clarify, healthcare organizations began partnering with data-handling specialists to manage their sensitive data. This partnership helped healthcare providers deliver medical care to patients more quickly and efficiently. However, the old HIPAA rules failed to ensure the safety and security of these third-party organizations that handle PHI.
So, to address growing gaps and unify changes under one rule, HHS issued the HIPAA Omnibus Final Rule in 2013. It brought several improvements and changes to the existing HIPAA privacy and security rules. To add on, the HITECH act widened the definition of business associates, bringing many business entities under the HIPAA regulations. The act also increased the penalties for HIPAA violations. They also passed the Genetic Information Nondiscrimination Act (GINA) to end the discrimination based on genetic data.
Eventually, all these regulations resulted in confusion and compliance issues for the healthcare business. Therefore, they passed the HIPAA omnibus rule to enhance and refine the existing HIPAA security rules. This rule expands the scope of the HIPAA Act, increases penalties for violations, grants patients more rights over their PHI, and introduces stricter breach notification requirements.
KEY CHANGES INTRODUCED BY THE HIPAA OMNIBUS RULE
The HIPAA Omnibus Rule changes, introduced in the HIPAA update of 2013, brought several major improvements. Here are the key updates that every healthcare organization and its business partner must know.
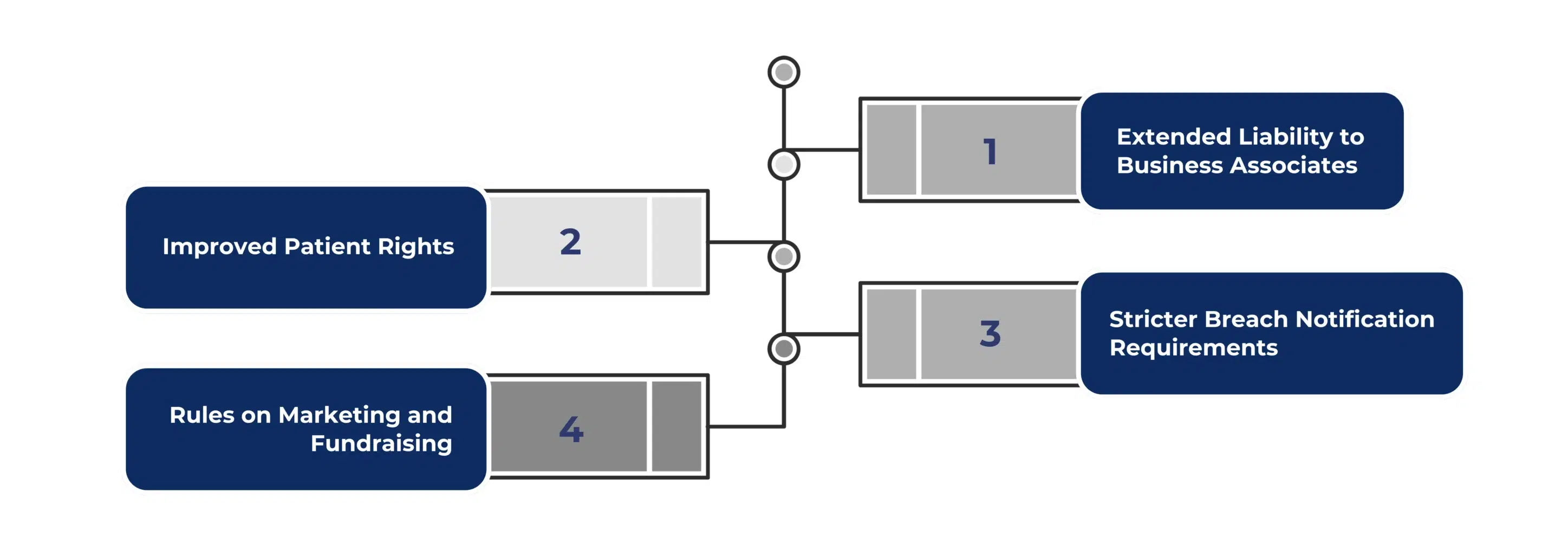
Extended Liability to Business Associates: One of the most important changes was the expansion of HIPAA compliance requirements to business associates. These are third-party vendors like billing services, cloud storage providers, and IT contractors. Before 2013, only healthcare providers and insurers had full responsibility to adhere to HIPAA rules. Now, under the business associate HIPAA responsibilities, these vendors must also protect patient data as per the HIPAA omnibus rule.
Improved Patient Rights: The HIPAA omnibus rule also gave more power to patients. Now, individuals can request copies of their medical records. Plus, they can also direct providers to send this data to a third party. Another key right allows patients to limit the disclosures to health plans if they cover their treatment expenses. As a result, the HIPAA omnibus final rule improves transparency and gives patients more control over their information.
Stricter Breach Notification Requirements: Under the omnibus rules HIPAA, organizations must report any data breach unless they can prove there is a low chance of harm. Prior to the omnibus HIPAA final rule, only a data breach affecting 500 or more people was supposed to get an official breach notification alert. This situation was changed and gave more flexibility to the rules. Now, covered entities must evaluate and document every breach carefully. This change has promoted faster action and more accountability.
Rules on Marketing and Fundraising: The HIPAA omnibus rules also tightened the rules around marketing and fundraising. Accordingly, the covered entities must now get patient authorization before using health data for these purposes. This change has helped prevent the misuse of private information and protect patient trust.
WHO NEEDS TO COMPLY WITH THE HIPAA OMNIBUS FINAL RULE
First of all, the belief that HIPAA rules are just meant for hospitals and doctors is a misconception. And it must be clarified. Because the HIPAA omnibus rule has changed the situation now. The reach of HIPAA rules now covers more than the traditional healthcare providers. With this upgrade, now anyone who touches the PHI must achieve compliance with omnibus rules HIPAA.
The primary players who need to comply with HIPAA omnibus rule are the covered entities. They are your core healthcare providers like hospitals, private clinics, pharmacies, dentists, and insurance providers. In simple words, if you deliver healthcare, process medical claims, or deal with patient records as your main operation, then you are a covered entity.
Then come the business associates. These are companies or individuals that help covered entities while handling PHI. They include IT support teams, billing services, cloud storage providers, and even SaaS tools for appointment scheduling. If these companies or individuals manage or store PHI, even for a temporary period, they are now accountable for following HIPAA regulations.
Now, here is where the HIPAA omnibus rule gets trickier. Have you heard about the subcontractors? They are the contractors who work for the business associates. For instance, if a billing firm hires a third-party data processor, then that subcontractor also possesses the same HIPAA responsibilities now. The subcontractors cannot ignore their HIPAA responsibilities by claiming that they have not yet spoken with any patients.
Thus, the HIPAA omnibus rule has fixed the loopholes in previous regulations. Now, no business could ignore it by saying, “We didn’t know.” Your business must adhere to the HIPAA regulations whether it handles PHI directly or indirectly. Everyone in the sensitive medical data chain is now visible and liable under the omnibus rules HIPAA.
BEST PRACTICES TO STAY COMPLIANT WITH THE HIPAA OMNIBUS FINAL RULE
The HIPAA omnibus rules have a major impact on your organization’s HIPAA compliance strategy. So, to stay compliant, you must implement certain changes to your approach. The first step is to update your Business Associate Agreement (BAA). Make sure that they provide a proper definition for the roles and responsibilities of every party involved in the compliance process. As the business associates are liable for HIPAA rules, your BAA must reflect this change accordingly. The next step is to update your internal policies in accordance with the amended HIPAA privacy and security rules. This also includes your firm’s breach response policy. You must now evaluate each incident and report it, regardless of the number of individuals affected.
Also, keep in mind that the penalties for non-compliance could reach up to 1.5 million dollars per year. Ignoring HIPAA regulations could therefore be harmful to your financial stability, reputation, and trust. With regard to the above-mentioned information, there are certain best practices that healthcare businesses must follow. The following best practices help them in staying compliant with the HIPAA omnibus rule:
Regular Risk Assessments: Have a regular review of your assets, such as systems, clouds, and data. This helps you identify where your patient data is stored and how it is shared. This helps you to spot weaknesses and gaps hidden inside your system.
Implement Audit Trails: Maintain a proper record of who accesses what and when. These digital footprints could help you find unusual activities easier. Moreover, audit trails serve as your proof of compliance during external audits.
Set Access Controls: Encrypt your data using strong passwords, role-based access controls, and multi-factor authentication.
Documentation and Training: Update your policies and document all compliance activities regularly. With this, you ensure that only authorized people gain access to PHI.
SECURE YOUR HIPAA COMPLIANCE WITH CERTPRO BY YOUR SIDE
We recognize that healthcare businesses and startups face numerous challenges. This includes taking care of patients, providing timely healthcare, and doing the paperwork, all with a limited budget and resources. At the same time, even one error in handling PHI will cost you millions along with your trust. Each and every form, email, and system you handle must be secure.
And with the HIPAA omnibus rule, now it’s not just the duty of covered entities to comply with HIPAA rules. The business associates, the subcontractors, and anyone who handles Protected Health Information (PHI) must follow the HIPAA regulations. If your business handles health records, the omnibus rules of HIPAA apply to you too.
But you don’t have to do it alone. CertPro steps in to take care of your HIPAA compliance journey. We don’t act just as your compliance consultant. Rather, we work along with you as your trusted partner and valuable guide. Our audit team assists you in understanding everything from rewriting BAAs to updating your risk strategies. Contact CertPro today to build a strong HIPAA compliance strategy that fits your size and budget. Together we could build trust and a secure future for your healthcare business.
FAQ
What is the purpose of HIPAA omnibus rule?
The primary purpose is to strengthen the security of sensitive health data, particularly in digital formats, and to grant patients greater access to their personal medical details.
What is the HIPAA privacy rule?
The HIPAA privacy rule establishes national standards to protect individuals’ medical records and other individually identifiable health information.
What are the three major types of HIPAA rules?
The three major HIPAA rules are the HIPAA privacy rule, the HIPAA security rules, and the HIPAA breach notification rule.
What are PHI data examples?
Examples of PHI data include the patient’s phone number, email address, social security number (SSN), and electronic medical record.
Who enforces the HIPAA regulations?
The U.S. Department of Health and Human Services (HHS) Office of Civil Rights (OCR) is responsible for enforcing the HIPAA privacy and security rules.

About the Author
BENEDICT ESSANDOH
Benedict Essandoh, CertPro’s Regional Director in Ghana, is a compliance and ISO standards expert. Specializing in health and safety, he conducts audits, implements ISO 9001 and ISO 45001, and excels in accident investigation and site inspections, ensuring international standards are met.
GRC IN CYBERSECURITY: WHAT IT MEANS AND WHY IT MATTERS IN 2026
In 2026, the pressure on companies to manage cyber risk responsibly has never been greater. Regulators demand structured controls, boards want clear risk reporting, and threat actors are becoming more sophisticated. Against this backdrop, GRC in cybersecurity has...
HOW COMPLIANCE AUDIT SOFTWARE IMPROVES AUDIT READINESS
Today, most companies deal with a growing number of compliance regulations. From data privacy standards to security frameworks like SOC 2 and ISO 27001, the list of compliance obligations keeps expanding. At the same time, regulators and external auditors now expect...
Compliance Best Practices in 2026: How to stay ahead of regulatory changes
Why is the implementation of compliance best practices critical for 2026? Compliance in 2026 demands operational proof, not the documentation intent. Regulations change faster, audit scrutiny is higher, and reporting timelines are tighter across privacy,...





