According to Reuters’ recent analysis, there is an alarming rise in exposed PHI caused by vendor and third-party system misconfigurations, poor encryption, and missing Business Associate Agreements (BAA). This proves that HIPAA violations in 2026 need not necessarily be headline-making incidents to cause damage. One small misstep, like a wrong email, is enough to attract penalties and damage your reputation. For instance, imagine your staff member has mailed a spreadsheet with patients’ Social Security Numbers to a vendor without encryption. Despite having no malicious intent, this incident will result in a HIPAA breach and fines.
So, what are “HIPAA Violations” in 2026? They’re no longer just about lost paper files or someone spying on a neighbor’s health record. With evolving regulations, increased oversight, and sophisticated cyber threats, violations now encompass weak security controls, careless vendor contracts, failure to report breaches on time, and misuse of newer technologies like cloud storage or AI.
Do you think that this only matters for healthcare providers? If yes, then you are wrong. To clarify, covered entities like healthcare providers, health plans, business associates, third-party vendors, and even staff in the back office will fall under the scope of HIPAA requirements. This is because mistakes could emerge from any point. Irrespective of whether you are sending bills with patient information or providing SaaS that touches PHI, you are obliged to follow the HIPAA rules and regulations.
In this blog, we offer expert guidance to avoid the pitfalls staff often stumble into and the vendor risks many companies underestimate. We help you understand where mistakes happen most, what vendors tend to get wrong, and how you can build systems to catch and mitigate even the minor issues before they escalate.
HIPAA VIOLATIONS IN 2026: AN OVERVIEW
TYPES OF HIPAA VIOLATIONS: CIVIL vs. CRIMINAL IN 2026?
WHAT ARE THE COMMON STAFF MISTAKES LEADING TO HIPAA VIOLATIONS?
HIPAA VENDOR COMPLIANCE: COMMON PITFALLS AND HOW TO GET IT RIGHT
BEST PRACTICES TO PREVENT HIPAA VIOLATIONS
Tl; DR:
Concern: HIPAA violations in 2026 extend beyond lost files or unauthorized data access. Today, they include vendor misconfigurations, missing BAAs, weak encryption, and delayed breach reporting. Regulators like the OCR have intensified enforcement, with over 725 major breaches reported in 2024 alone.
Overview: The biggest risks come from two fronts, namely staff mistakes and vendor failures. A single misaddressed email, shared login, or misconfigured cloud bucket can expose thousands of patient records. Remote work, AI-driven phishing, and complex subcontractor chains have expanded the attack surface, leaving compliance teams struggling to keep up. Reviewing real HIPAA violation examples shows how even mid-sized providers end up with six-figure settlements and public reputational damage.
Solution: The solution is proactive action. Conduct risk assessments frequently, not just annually. Audit vendors, enforce BAAs, and train staff with real-world scenarios. Implement strong access controls, encryption, and clear breach response plans. Partnering with experts like CertPro helps close compliance gaps faster. CertPro’s audits and compliance automation tools help you meet HIPAA standards, avoid costly penalties, and protect patient trust before a regulator knocks on your door.
HIPAA VIOLATIONS IN 2025: AN OVERVIEW
HIPAA enforcement has become far more active in 2026. The Office for Civil Rights (OCR) has issued updated guidance that stresses the need for risk assessments, timely breach notifications, and vendor oversight. Furthermore, the regulators now enforce stricter accountability regardless of intent. For instance, let’s say you are a mid-sized clinic with no history of security breaches. Yet, failing to sign proper Business Associate Agreements (BAAs) will be considered a HIPAA violation.
Additionally, the threats are also evolving. The boundaries between secure and risky environments are becoming increasingly blurred due to remote work. This is to say that staff might check patient records on personal devices, which often lack encryption or monitoring. Although cloud services enhance efficiency, misconfigurations can leave data vulnerable. Organizations should review real HIPAA violation examples to understand how simple mistakes can cause reportable breaches. Likewise, phishing attacks have become smarter with AI-generated emails that mimic internal staff language. Furthermore, third – party services dealing with PHI expand the attack surface, making vendor risk management critical.
The four main issues focused on by the OCR are vendor non-compliance, improper disposal of PHI, unauthorized access to patient records, and failure to perform risk assessments. These are not abstract problems. They are happening in real time. For example, the HIPAA journal states that, “By January 28, 2025, OCR had recorded 725 data breaches in 2024 where 500 or more records were exposed. This is the third year in a row that the number of major breaches has topped 700.” Reviewing HIPAA violation examples from past years shows that even mid-size practices face large settlements. The impact of violations goes well beyond fines. To elaborate, the financial losses could drain budgets for years, but reputational harm will lead to loss of patient trust. As a result, legal actions follow, dragging leadership into public scrutiny.
TYPES OF HIPAA VIOLATIONS: CIVIL vs. CRIMINAL IN 2026?
HIPAA violations are usually divided into two broad categories, civil and criminal. Civil violations happen when an organization slips up. This means they are unaware of the breach, or their safeguards were not strong enough. On the other hand, criminal violations involve intent. To clarify, someone intentionally knew that they were violating the rules and acted anyway.
Civil violations are far more common. For instance, examples of civil HIPAA violations include an employee faxing lab results to the wrong clinic, IT teams skipping a required risk analysis, and records being kept in an unsecured storage room. These aren’t malicious acts, but they still break HIPAA rules and can trigger HIPAA violation penalties for employees when reported.
Conversely, criminal violations are much more serious. These include incidents of selling patient data on the dark web, using PHI to commit fraud, or spying on a celebrity’s record out of curiosity. These cases go to the Department of Justice (DOJ) and lead to hefty fines and 10 years of imprisonment. Understanding HIPAA violation penalties for employees helps organizations set up proper training and monitoring programs to reduce risks.
Penalties for HIPAA Violations:
Civil Penalty Tiers:
- Tier 1: This category applies to genuine accidents that organizations are unaware of.
- Tier 2: This is when the organization should have known about the violation, but it did not due to willful neglect.
- Tier 3: Incidents where organizations violated the rules by willful neglect but corrected within the required time frame.
- Tier 4: HIPAA regulations were violated by willful neglect and not corrected, triggering the highest possible fines per violation.
Criminal Penalty Levels:
- Basic Offense: Up to 1 year in prison and a $50,000 fine for knowingly accessing PHI without authorization.
- False Pretenses: Up to 5 years in prison and a $100,000 fine for using deception to obtain PHI.
- Intent to Profit or Harm: Up to 10 years in prison and $250,000 for selling, misusing, or exploiting PHI for gain.
A clear understanding of HIPAA violation penalties for employees ensures that compliance leaders can create policies that prevent both accidental and intentional breaches.
WHAT ARE THE COMMON STAFF MISTAKES LEADING TO HIPAA VIOLATIONS?
Staff mistakes remain the single biggest driver of HIPAA violations. Most breaches emerge from everyday business activities. Human error and negligence are the first culprits. Indeed, a single misaddressed email could put sensitive data in the wrong hands. Similarly, unencrypted devices, when lost, turn into massive breach reports overnight. Inadequate training is another quiet risk. Many organizations conduct one-time onboarding sessions and then move on. However, ensuring compliance is not a one-time event. Without refresher training or scenario-based exercises, staff simply forget what are HIPAA violations and what’s at stake. Such forgetfulness could lead to mistakes during high-pressure scenarios and events involving workflow changes.
Weak access controls, such as shared logins, delayed offboarding, and excess privilege, create security gaps. If your former employee could still log into your system, you’re already under OCR investigation. Not to forget, the paper records are often overlooked. Unlocked file cabinets, documents left in common areas, or disposing of records in regular trash are still major causes of HIPAA violations. Compliance officers encounter these genuine challenges on a daily basis. But they are preventable with training, regular internal audits, and a culture that values patient privacy.
HIPAA VENDOR COMPLIANCE: COMMON PITFALLS AND HOW TO GET IT RIGHT
Third-party vendors could be both a lifeline and the weakest point of security for healthcare organizations. This means that even when your vendors mishandle data, your organization comes under HIPAA violations. That’s why vendor management has become one of the essential compliance challenges.
To add on, the most common mistake is missing or outdated Business Associate Agreements (BAAs). Some organizations still work with vendors without formal agreements or rely on generic templates that don’t satisfy security obligations. The HIPAA omnibus rule made BAAs even more critical by clearly defining vendors’ liability for protecting patient data. Therefore, as coveted entities, you must understand that if your vendor suffers a breach, you’ll be the one answering to the Office for Civil Rights (OCR). Then there’s the issue of vendor risk assessments. Too many compliance teams rely solely on vendor assurances. They trust claims of “HIPAA-compliant” software without verifying. Always consider a thorough risk assessment to check whether vendors encrypt data, patch vulnerabilities, and train their staff.
Data handling mistakes are another big trigger for HIPAA violations. For instance, your vendors sometimes send unencrypted files over email, misconfigure cloud storage, or leave sensitive data exposed. Cloud and software providers are particular obstacles to HIPAA compliance. Because your IT team thinks the vendor handles security, while the vendor assumes you’ve configured privacy controls. This shared responsibility gap is where HIPAA breaches happen.
In the end, please bring your subcontractor chains to the security radar. To elaborate, if your vendor uses another vendor and fails to sign BAAs or monitor them, it is one of HIPAA violation examples.
BEST PRACTICES TO PREVENT HIPAA VIOLATIONS
In this section, let’s understand the practical controls and best practices that your organization could implement to prevent internal staff errors and vendor mistakes.
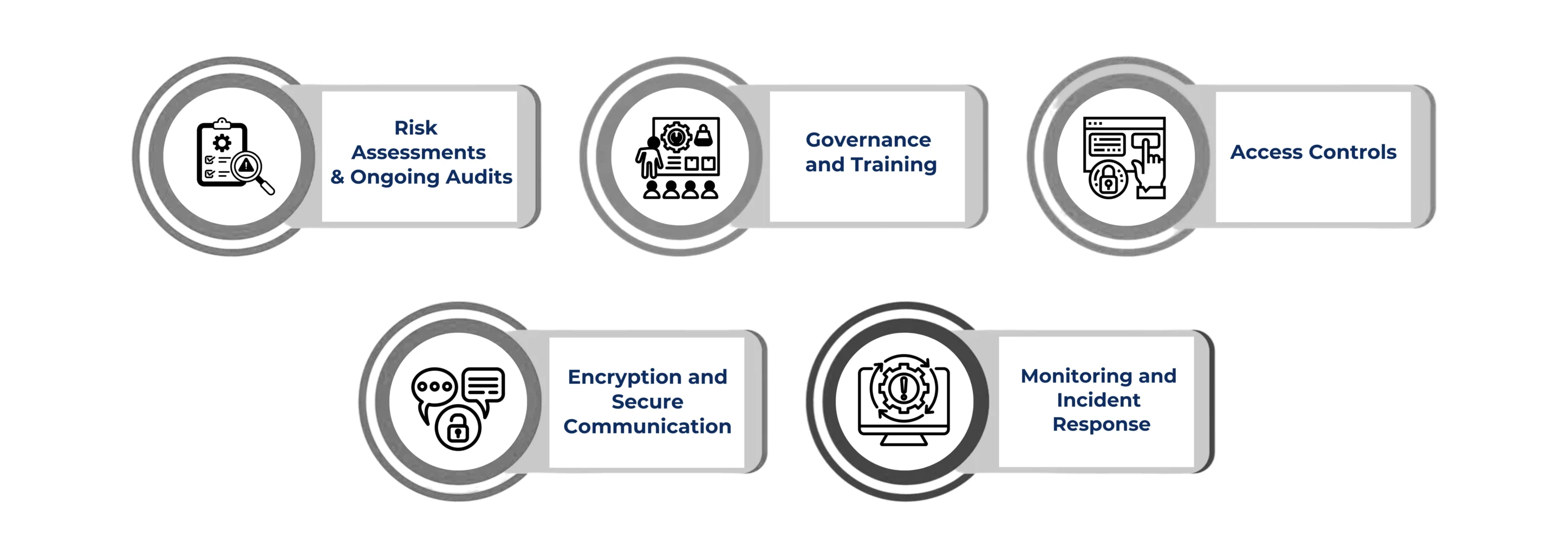
Risk Assessments & Ongoing Audits: A solid HIPAA compliance program needs regular internal audits and vendor risk assessments rather than running on autopilot mode. Instead of following an annual audit schedule, conduct regular checks and reviews. This procedure includes incidents like adding new software, onboarding a vendor, or changing a workflow. Verify everything from your servers, laptops, physical security, and even vendor contracts. Never rely solely on your security measures. One internal audit is enough to identify issues such as weak access controls and a lack of encryption.
Governance and Training: Ensure that Policies are simple enough that your staff can actually follow them without any confusion. Furthermore, update them regularly and ensure routine training sessions. For example, Scenario-based sessions work best. Therefore, consider involving people in simulation training and incident response drills.
Access Controls: This is another area where things can become messy. Therefore, ensure that each individual has their own login, accompanied by role-based access controls. And revoke accounts the minute someone leaves.
Encryption and Secure Communication: Emails, file transfers, and even trash disposal need a proper SOP. If you fail to adhere to a proper PHI disposal policy, you may find yourself under OCR’s scrutiny.
Monitoring and Incident Response: Establish a proper policy on who gets reported first during security incidents, and consider proper documentation of their response and mitigation efforts.
CERTPRO IS YOUR STRATEGIC HIPAA COMPLIANCE PARTNER
HIPAA violations are no longer a distant legal problem. It has become a real business challenge that shows up in contracts, cloud settings, and everyday tools. Regulators are now running targeted audits and releasing stricter guidance on vendor oversight and risk analysis. At the same time, vendors and system misconfigurations remain a frequent cause of patient data exposure, making accountability harder to ignore. Furthermore, the financial impact of a single breach can reach millions, and delaying action only increases the cost and the recovery time.
This is where CertPro becomes your strategic partner in HIPAA certification and compliance. Our team exactly knows what are HIPAA violations. Thus, we identify the real gaps, such as outdated contracts, cloud misconfigurations, and weak offboarding processes. We ensure that you adhere to all HIPAA regulations that are relevant to your business nature and scope. Hence, taking action now reduces the chance of a breach, protects patient trust, and prevents legal battles.
If you want focused guidance on HIPAA compliance, connect with CertPro today. We use quality audits and market-leading compliance automation tools to help you achieve HIPAA compliance with ease. This helps you in staying ahead of risk and promises long-term business growth.
FAQ
What is the most common HIPAA violation?
The most common HIPAA violation is human error, such as misaddressed emails, lost unencrypted devices, or unsecured paper records. These mistakes often expose patient health information (PHI) and lead to investigations, fines, and mandatory corrective actions from regulators.
What qualifies as a HIPAA breach?
A HIPAA breach happens when protected health information (PHI) is accessed, shared, or exposed without proper authorization. This includes hacking, snooping, lost devices, vendor errors, or misdirected communication that risks patient privacy or security.
What are the consequences of a HIPAA violation?
Consequences include tiered fines ranging from hundreds to thousands of dollars per violation, possible criminal charges, and loss of reputation. Organizations may also face lawsuits, costly breach notifications, and mandatory corrective action plans from the Office for Civil Rights.
Who must comply with HIPAA?
HIPAA applies to covered entities like healthcare providers, health plans, and clearinghouses, as well as business associates that handle patient data. This includes software vendors, billing services, and any third party with access to PHI.
What are Business Associate Agreements (BAAs) in HIPAA?
A BAA is a legally required contract between a covered entity and a vendor that handles PHI. It defines each party’s security responsibilities and ensures the vendor follows HIPAA standards for data privacy and breach reporting.

About the Author
Abhijith Rajesh
Abhijith Rajesh is an Associate Manager at CertPro, specializing in ISO 27001, SOC2, GDPR, and other Information Security Compliance standards. He leads a dedicated team, ensuring the delivery of top-tier information security solutions. Abhijith excels in managing projects, optimizing security frameworks, and guiding clients through the complexities of the ever-evolving threat landscape.





